Venous Insufficiency
What is the Venous System?
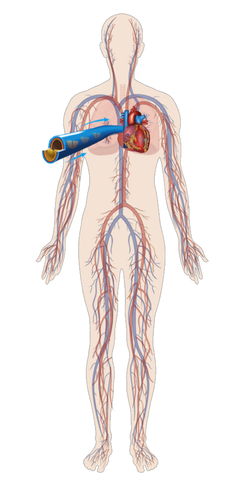
Venous simply means relating to the veins. The venous system is the network of veins responsible for transporting de-oxygenated blood from various regions in the body back to the heart. This blood is then re-oxygenated before being returned back into circulation.
Blood needs to move from the legs back up to the centre of the body. To ensure it can only go up instead of down, veins contain valves. The veins and valves need to be a good condition in order for the Venous System to work efficiently.
What is Chronic Venous Insufficiency?
Chronic Venous Insufficiency (or CVI) occurs when the venous wall and/or valves aren’t working properly. This makes it difficult for blood to return to the heart and it pools in the lower legs, causing swelling.
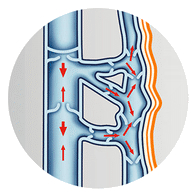
What is Chronic Venous Insufficiency (CVI)?

Overview
It is estimated that by the age of 50, nearly 40% of women and 20% of men have significant problems with the veins in their legs and are living with Chronic Venous Insufficiency.
Often, older people who have developed CVI will have chronic odema (swelling) as a result from being less mobile. If this persists for more than three months, it is classed as phlebolymphedema, from the Greek ‘phlebo’, which translates as ‘vein’ and ‘odema’, meaning ‘swelling’.
The good news is, with the right support and treatment, your symptoms can be managed at home and you can avoid serious problems, which can develop if left untreated, such as leg ulcers.
There are two main ways of formally diagnosing Chronic Venous Insufficiency: Duplex Ultrasound and Magnetic Resonance Venography (MRV).
Duplex Ultrasound uses both a transducer and a probe to understand how the blood circulates and the structure of leg veins.
Magnetic Resonance Venography (MRV) uses a combination of a large magnet, radio frequencies and a computer to produce detailed images of the body’s organs and structures.
Both are painless procedures and don’t take a long time to undergo. Your care provider will put you at ease during your examination.
If you develop lymphedema as a result of Chronic Venous Insufficiency, any wounds and ulcers in the affected area will take longer to heal. This is because blood flow to the wound site is compromised and odema (the fluid that has accumulated in the surrounding tissues) blocks the flow of nutrients to and from the affected area.
You are also at risk of certain infections:
- Cellulitis – A bacterial skin infection which can occur in an area of untreated edema and makes the skin look red, feeling hot or painful to the touch.
- Erysipelas – An infection with a distinctive rash that also causes redness, swelling and warmth
- Both Cellulitis and Erysipelas, if untreated, can cause systemic infection making you feel unwell with a raised temperature
- Fungal infections – Often develop in skin folds or between your toes
- Lymphangitis – is an infection of the lymph vessels beneath your skin that makes your lymph nodes feel swollen and tender
It’s important to keep an eye on any changes in your body to prevent potentially serious infections from developing. It might help to keep a diary of your condition and show it to your care provider.
While there are reasons you might be more likely to develop Chronic Venous Insufficiency, there many things you can do to help prevent it:
- Get medical support to stop smoking
- Try to exercise regularly
- Avoid prolonged periods of standing or sitting
- Eat a well-balanced diet
- Ask for help to lose weight, if you're overweight
- Wearing support/compression stockings
If you think you might be at risk for CVI, ask your medical professional before making any of these changes.
Symptoms
Everyone’s symptoms are different and will be more, or less, severe, depending on the stage of their condition. Here are some symptoms to look out for:
- Swelling in the lower legs, especially after prolonged sitting or standing
- Swelling that progresses over time
- New varicose veins
- Aching, heaviness, or tiredness in the legs
- Flaky or itchy skin of the legs
- Skin of the legs appears leathery
- Venous stasis ulcers (common in the inside area above the ankle) These shallow red sores occur when blood has pooled in the legs and remains static
- Leg cramps
Causes
While anyone can develop Chronic Venous Insufficiency in their life, there are several risk factors that may make it more likely to develop:
- Deep Vein Thrombosis (DVT)
- venous hypertension
- Varicose Veins/CVI
- Pregnancy
- Obesity
- Smoking
- Inactivity
- Prolonged periods of sitting or standing
- Hormonal changes
- Female sex
- Age over 50
- Family history
Stages
There are three different stages (according to Widmer) of CVI, ranging from mild to more severe symptoms.
Swelling and pigmentation
In mild CVI, symptoms come and go. Swelling may reduce when the limb is elevated. It usually involves the ankle and calf.
Management: Compression and advice on how to look after your skin.
Swelling, skin pigmentation, and dermatitis.
Moderate CVI starts to affect the foot and toes, as well as the ankle and calf.
Management: Compression, skin care advice, and possibly a vascular consultation.
Swelling, varicose veins, skin pigmentation, dermatitis, and ulceration.
Severe CVI causes more skin problems and ulcers, in addition to swelling.
Management: Compression; ulcer care plan, and possibly a vascular consultation.